How Common is Fecal Incontinence ?
It is estimated that 2 to 7 percent of the general population has fecal incontinence. In the United States alone, more than 5.5 million suffer from fecal incontinence. Although the actual number may be more as many people have difficulty talking about this problem with their doctor. Fecal incontinence is more common in older people and in women.
Symptoms of Fecal Incontinence
People suffering from fecal incontinence pass their stools or gas without their control. This spoils their clothes and surroundings. Normally fecal leakage should not happen in adults except during episodes of severe diarrhea. Fecal incontinence can range from mild to severe. In mild cases, you may only have difficulty controlling gas, while in severe cases, you involuntary pass formed stools. Other symptoms include:
- Urgency
- Abdominal discomfort
- Bad odor
- Diarrhea or constipation
- Anxiety
Causes of Fecal Incontinence
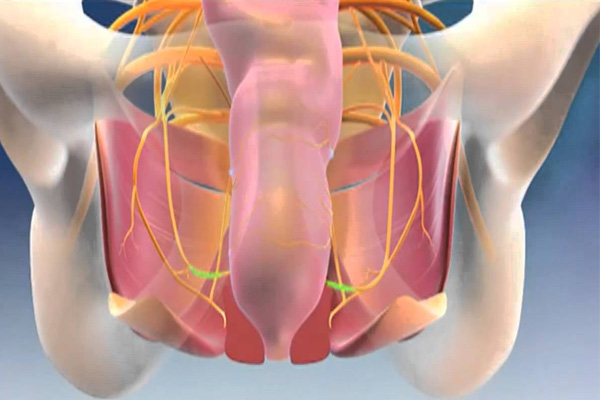
Normally, the lower part of our intestine, rectum, anus along with our nervous system have to be working fine to control the bowel movements. We have a group of muscles called sphincters that control and hold stool, when surroundings are not convenient to pass the bowel movement.
Fecal incontinence is commonly caused by abnormal sphincter function or damaged nerves supplying the sphincter and other muscles. This damage may occur during child birth in women, during anal surgery, after trauma, stroke or in patients with uncontrolled diabetes mellitus.
Risk Factors of Fecal incontinence
Fecal incontinence is more commonly seen in older people and in women. They often have a history of:
- Multiple pregnancies and vaginal deliveries
- Complicated childbirth
- Anal surgery
- Stroke
- Multiple sclerosis
- Advanced dementia
- Uncontrolled diabetes mellitus
Complications of Fecal Incontinence
- Bad odor
- Infections
- Anxiety or depression
- Social isolation
Diagnosis of Fecal Incontinence
Your doctor will first take a detailed history and will perform the relevant physical examination. Your doctor may also perform a digital rectal examination (DRE). It is a simple bedside procedure in which your doctor will insert a gloved finger into your anus to look for any abnormality or weakness in the anterior wall of rectum.
Your doctor may also advise for additional tests including:
- Proctosigmoidoscopy to visualize rectum and anus.
- Anal manometry to measure the strength of the anal sphincter.
- Defecography that includes a series of x-rays to see the bowel movements.
- Anal electromyography (EMG) to identify nerve damage in your anus.</li
- Ultrasound scan, computerized tomography (CT) scan, or magnetic resonance imaging (MRI).
Treatment of Fecal Incontinence
Treatment of fecal incontinence depends upon the underlying cause and severity. Multiple conservative and surgical treatment options are available. Your doctor will discuss different treatment methods and will guide you accordingly.
Conservative management includes:
- Preventing constipation by dietary changes and stool bulking forming medicines.
- Anti-diarrheal medicines if diarrhea is the main cause for fecal incontinence.
- Muscle strengthening exercises.
- Biofeedback
- Surgical Management of Fecal incontinence
Different surgical options are available to treat fecal incontinence, again depending upon the cause and severity of your condition. Some of these procedures can be performed through the abdomen and others are performed through anus. Your doctor will discuss these options with you and advise you according to your general health and your condition. General anesthesia is often required for these procedures. Surgical options include: - Anal muscle repair
- Stimulation of the nerves
- Bulking agent injections
- Colostomy
Follow Up
After surgery, you will be given optimum pain killers. You should avoid sexual intercourse till the wound heals. Your doctor will give you follow up appointment, usually after 1-2 weeks. You may also be advised for regular dressings till wound heals. You are advised to follow your doctor’s instructions. Notice for any signs of infection, such as a fever, tenderness, swelling, or redness. If you experience any of these signs, you should contact your doctor immediately.