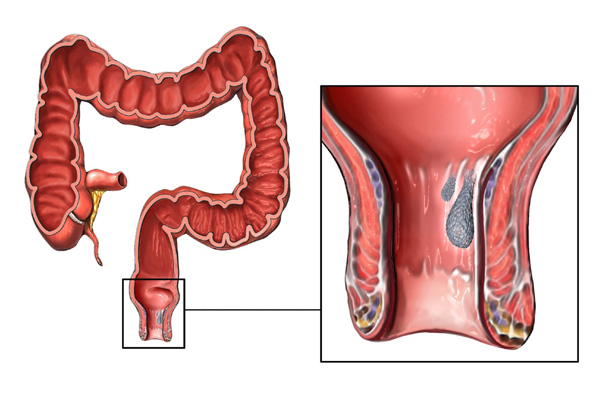
What is Rectal Prolapse?
The rectum is a small part of your lower large intestine, measuring only a few inches.
Rectal prolapse is a medical condition in which the rectum extends outside the anus. Rectal prolapse mostly affects adults and is more common in women than men.