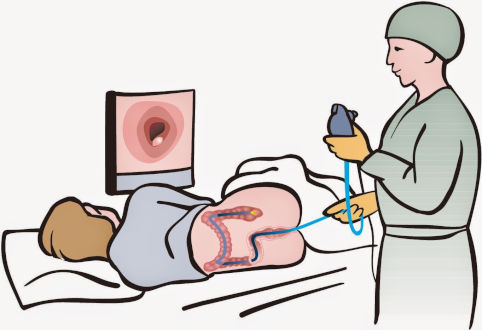
Colonoscopy
A colonoscopy is a diagnostic procedure performed to examine the inside of the colon and rectum. The colonoscopy procedure is performed to determine the cause of changes in bowel activity, abdominal pain, or rectal bleeding, as well as to detect early signs of cancer.