What is Crohn’s Disease?
Crohn’s disease is a chronic inflammatory condition of the digestive tract. It is one of the two types of inflammatory bowel disease (IBD), the other being ulcerative colitis. The disease is named after Dr. Burrill B. Crohn.
Crohn’s disease is a chronic inflammatory condition of the digestive tract. It is one of the two types of inflammatory bowel disease (IBD), the other being ulcerative colitis. The disease is named after Dr. Burrill B. Crohn.

The most common symptoms of Crohn’s disease are:
In Crohn’s disease, symptoms are intermittant. Sometimes, they are very severe (this is called a “flare-up”). At other times, you may be completely symptom-free, in “clinical remission”.
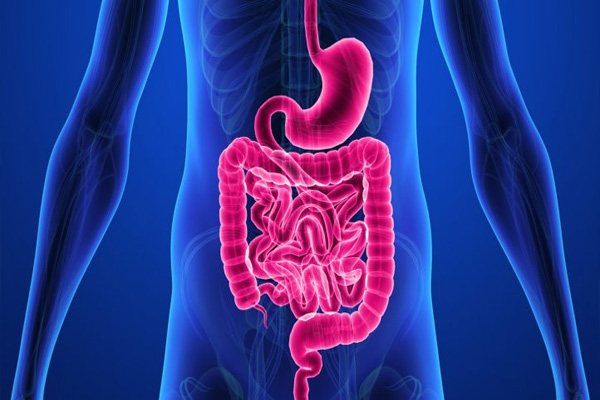
Crohn’s disease is an autoimmune disease, in which your body’s immune system recognizes the lining of your digestive tract as a foreign body and attacks it, causing inflammation. This inflammation results in ulcers and bleeding. The exact cause that triggers our immune system to attack our own cells is mostly unknown. Crohn disease usually affects the last part of the small intestine (called the “ileum”) and some of the large intestine (colon) but it can affect the entire digestive tract, from the mouth to the anus
Risk factors for Crohn’s disease include:
Crohn’s disease may lead to one or more of the following complications:
Your doctor will first take a detailed history and perform the relevant physical examination. Since multiple other conditions can produce the same symptoms as Crohn’s disease, your doctor will suggest various medical tests to confirm the diagnosis. Tests may include:
There is no complete cure for Crohn’s disease but multiple medicines are available that help to reduce the symptoms of Crohn’s disease. The groups of medicine commonly used to treat Crohn’s disease are:
Almost all of these medicines work by reducing inflammation and the body’s immune response. Every person has a different response to their medicines. Your doctor will advise for these medicines depending upon your general health and symptom severity. Your doctor may also sometimes prescribe antibiotics during flare up or with anal discharge. You might have to try a few different medicines before you find the one that works best for you.
Awareness of the diet and a focus on nutrition may help to reduce the symptoms of Crohn’s disease by restoring nutrients that have been lost, and by encouraging the healing process. Restricting dairy products, and foods high in fiber and fat, may help to prevent flare-ups of the disease. Quitting smoking and reducing stress are also helpful. Surgical options include:
Although there is no clear evidence that foods actually cause inflammatory bowel disease, certain foods may aggravate your symptoms of Crohn’s disease. Your doctor may recommend a special diet given via a feeding tube (enteral nutrition) or nutrients injected into a vein (parenteral nutrition) to treat the symptoms of your Crohn’s disease. This not only improves your overall nutrition but also allows your bowel to rest. Bowel rest can reduce inflammation in the short term. Your doctor may also recommend: